Can one drive after having the OCT eye examination?
1. If it is a “non-mydriatic” examination (without dilating the pupils) - one can drive directly
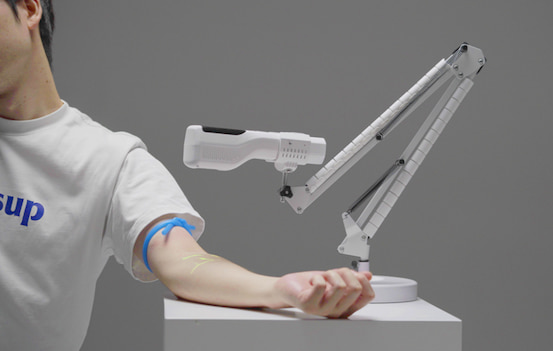
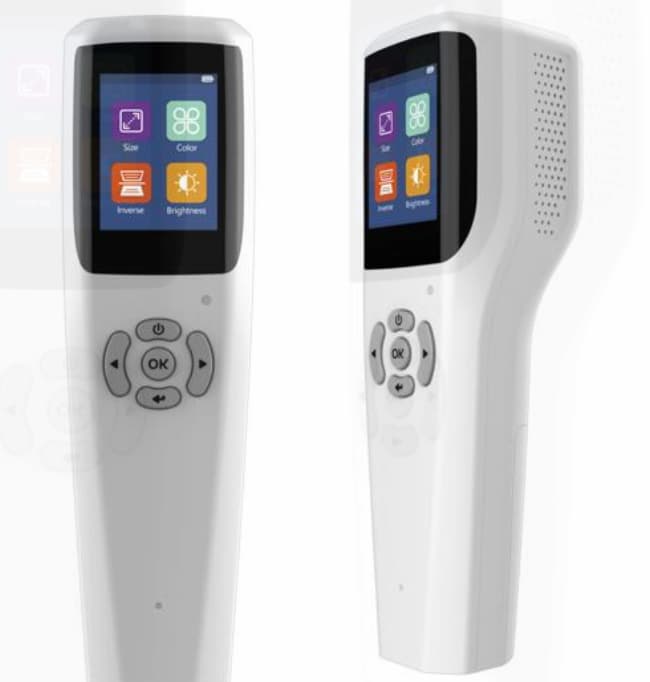
Many of the current high-end OCT devices (especially in routine screenings) have the feature of non-mydriatic examination. If the patient did not receive any eye drops to dilate the pupils before the examination, but simply looked at the cursor of the instrument for a while:
Visual status: After the examination, the vision is exactly the same as before the examination, with no blurriness or photophobia. Driving advice: You can definitely drive away by yourself right away.
2. If it is a "mydriatic" examination - absolutely not recommended for driving
If in order to observe the more peripheral areas of the retina, or if the patient's pupils are naturally too small, the doctor gave the patient mydriatic eye drops before performing the OCT:
Visual condition: After dilation, the patient's pupils will enlarge and lose their ability to adjust. This will result in blurred vision when looking at close objects (making it difficult to see the dashboard or a mobile phone), and extreme photophobia (if it's during the day, the sunlight outdoors or the car lights at night can be extremely bright, causing the inability to open one's eyes).
Driving advice: For safety, do not drive yourself at all. The effect of the mydriatic drugs usually takes 4 to 6 hours (or even longer) to completely wear off. Patients need to be picked up by relatives or friends, or take public transportation/take a taxi, and it is best to wear sunglasses to block the light when going out.
This device can help the clinic save the waiting time for eye dilation, enhance patient satisfaction (patients can leave immediately after the procedure, without affecting driving or daily life), and thereby achieve a higher daily check-up throughput.
Interested in becoming a distributor? Contact us for wholesale pricing.
Also welcome to contact us, we are ZD Medical Inc.
Tel : +86-187 9586 9515
Email : sales@zd-med.com
Whatsapp/Mobile : +86-187 9586 9515