1) Traditional Screening Methods and Their Limitations
Traditionally, the screening and staging of DR Mainly relied on color fundus photography to observe two-dimensional surface lesions such as retinal microaneurysms, hemorrhage and exudation. However, this method has limitations:
Strong subjectivity: Relying on the doctor’s experience.
Inability to observe deep structures: It is impossible to quantitatively assess the early structural damage of the retina, especially the early morphology of diabetic macular edema (DME).
2) The core role of OCT in the early detection of DR
OCT is a non-contact and non-invasive cross-sectional imaging technique, similar to “optical biopsy”, which can provide micrometer-resolution images of each layer of the retina. Its application in early DR Is mainly reflected in the following aspects:
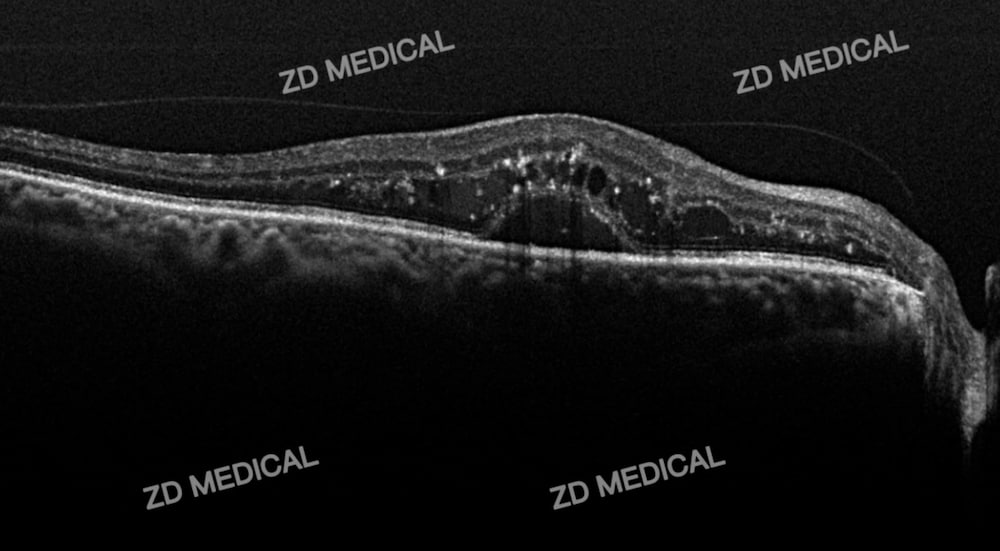
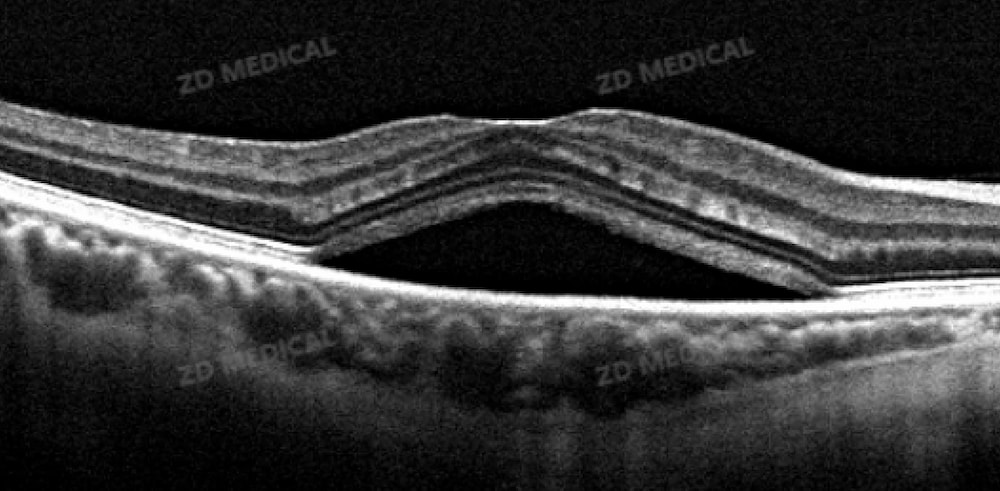
1. Detect subclinical diabetic macular edema
Key finding: OCT can detect before clinically visible retinal thickening or hard exudation (visible in traditional fundus photography) occurs in patients:
A slight thickening of the inner layer of the retina.
Early and local damage to the outer structures of the retina (such as the ellipsoid zone and the external membrane).
Tiny cystoid hyporeflex cavities (early cystoid edema).
Significance: This enables doctors to initiate or intensify treatment (such as optimizing blood sugar and blood pressure control, or considering early anti-VEGF therapy) before vision decline occurs, thereby protecting central vision.
2. Quantify the thinning of the retinal nerve fiber layer and ganglion cell layer
Key finding: DR Is not only a vascular disease but also a neurodegenerative disorder. OCT can precisely measure:
Retinal nerve fiber layer (RNFL) thickness: RNFL thinning can occur in patients with early-stage DR, which is related to the course of diabetes and blood glucose control.
Ganglion cell-inner plexiform layer (GC-IPL) thickness: This is a more sensitive indicator. Its thinning may occur earlier than microvascular lesions, suggesting early neuronal damage related to diabetes.
Significance: It provides objective biomarkers for the early neurodegeneration of DR, which is helpful for a comprehensive assessment of the condition.
3. Identify subtle vascular abnormalities and ischemiaOCT angiography (OCTA) : This is a revolutionary extension of OCT technology. Three-dimensional retinal and choroidal vascular maps can be generated without the injection of contrast agents.
Early detection: It can clearly show the expansion and irregular shape of the non-perfusion area (ischemic area), the avascular area of the fovea centrae in the macular region (FAZ), and the reduced density of the retinal capillary network. These changes may occur in the early stage of DR (even in the non-proliferative phase).
Advantages: Non-invasive, rapid and repeatable, it avoids the allergic risks associated with fluorescence angiography and is highly suitable for follow-up and monitoring.
4. Monitor the changes at the vitreoretinal interface
Key finding: Early DR May lead to abnormal adhesion or partial detachment of the posterior vitreous cortex (PVD), which is a risk factor for future traction, vascular rupture or macular edema. OCT can clearly display these subtle interface changes.
3) Summary of OCT Technology Advantages
High resolution and objective quantification: Provide objective and quantifiable data (thickness, volume, density), reducing subjective errors.
Non-invasive and fast: Highly accepted by patients, suitable for routine screening and frequent follow-up.
Three-dimensional and hierarchical analysis: It can precisely locate the level of the lesion in the retina.
Function Expansion (OCTA) : It has achieved non-invasive capillary-level blood flow imaging, significantly enhancing the ability to detect early ischemia and vascular abnormalities.
4) Application Paths in Clinical Practice
Screening stage: For all patients with type 2 diabetes and those with a longer course of type 1 diabetes, in addition to traditional fundus photography, OCT (especially macular OCT) should be included as part of baseline examination and annual screening when conditions permit.
Diagnosis and staging: When mild non-proliferative DR (NPDR) is detected by fundus photography, OCT can assess whether there is subclinical macular edema or thinning of the nerve layer, helping to conduct more precise risk stratification.
Treatment decision-making and follow-up: For patients who have developed DME or require panretinal photocoagulation, OCT is the gold standard tool for guiding treatment (anti-VEGF, laser) and evaluating efficacy. OCTA is used to assess the degree of ischemia.
Interested in becoming a distributor? Contact us for wholesale pricing.
Also welcome to contact us, we are ZD Medical Inc.
Tel : +86-187 9586 9515
Email : sales@zd-med.com
Whatsapp/Mobile : +86-187 9586 9515